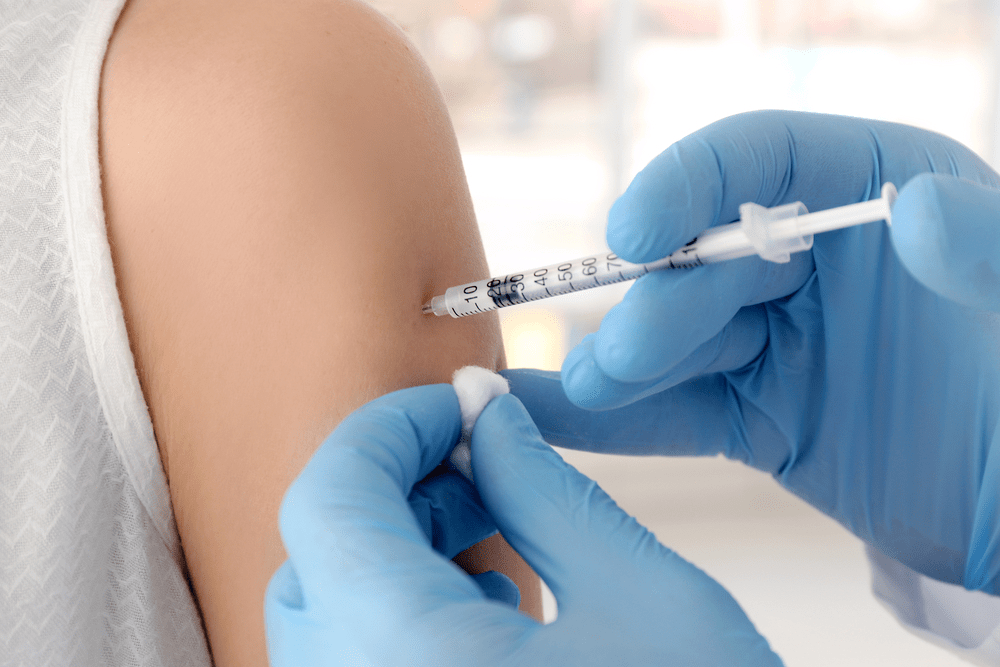
Vaccines are valuable discoveries in medicine, playing a significant role in protecting people’s health and eradicating diseases. While evidence of vaccinations exists from as far back as 1000 CE, it was not until Edward Jenner’s attempt to create smallpox immunity in 1796 did the practice gain major traction.
Since then, scientific research and technological advancements have enabled vaccination to protect people against many illnesses. These greatly contributed to the eradication of smallpox, with polio now reduced by 99% from the face of the earth.
This article aims to discuss the facts behind the different types of vaccines—how they work, how they are developed, and what makes them effective.
How Do Vaccines Work?
With a vaccine, antigens—molecules present in all forms of viruses and bacteria–are injected into the body. From there, the immune system identifies and combats them, storing the information about these invaders for the future. If the same bacteria or virus reappears, the immune system will easily recognize the antigens and attack the source before it spreads and causes illness.
Aside from being effective on an individual level, vaccination can serve as protection for entire populations. The more people in a population are immunized against a particular bacteria or virus, the fewer opportunities there are for an outbreak. This phenomenon is known as “herd immunity.”
This protection is critical for members of the population who cannot be vaccinated, such as the elderly, young children, people with severe allergies, and the immunocompromised. Through herd immunity, many infectious diseases have been eliminated without having to vaccinate every member of the population.
How Is Immunity Developed Through Vaccination?
There are different strategies employed to develop immunity, each with its own strengths and limitations.
1. Weakening the virus
Through this strategy, viruses are weakened to limit the spread of infection in the body. Due to the virus’s limited reproduction, the immune reaction is enough to induce memory B cells to protect against future infections without causing illness to the recipient. Vaccines for measles, mumps, rubella, rotavirus, chickenpox, and influenza were created through this method.
While a weakened strain provides almost life-long immunity, it can pose a high risk for people with a weak immune system.
2. Inactivating the virus
This strategy calls for completely inactivating, or “killing,” the virus through a process or with a chemical. This prevents it from reproducing or causing disease. When administered, however, the body can still detect the virus and generate the necessary antibodies to protect against the disease. Polio, hepatitis A, and rabies vaccines were made this way.
Inactivated vaccines cannot cause the diseases they prevent, making it safer to administer to individuals with weakened immune systems. The downside of this is that several doses are required to achieve immunity.
3. Using part of the virus or bacteria
This method uses certain components of viruses or bacteria that cause diseases, rather than as a whole. The vaccine may consist of a protein found on the virus’s surface, an inactivated toxin from a bacteria, or a bacteria’s polysaccharide coating. Vaccines for hepatitis B, human papillomavirus (HPV), diphtheria, tetanus, and pneumococcal were produced this way.
Like inactivated vaccines, these options are safer for people with weakened immune systems. They also require more doses to ensure continuous immunity.
The Process of Developing a Vaccine
Before a vaccine can be sold in the market and administered to the public, it undergoes a long research and testing process.
1. Exploratory Stage
Intensive research is done—usually taking 2–4 years—to identify the natural or synthetic antigens to help prevent or treat a certain disease. These antigens may include weakened strains of the virus itself, virus-like particles, weakened bacterial toxins, and other substances derived from the pathogen.
2. Pre-Clinical Stage
Once the research is complete, the candidate vaccine will be tested to determine its immunogenicity, or the ability to produce immunity. This stage is also used to test its general safety for the vaccine recipient. Cell-and-tissue culture systems and animal testing are used to help scientists get an idea of the possible cellular response in humans. This stage normally takes 1–2 years.
3. Clinical Development
If the candidate vaccine passes the pre-clinical stage, a sponsor—often, a private company—will submit an application for an Investigational New Drug (IND) to the U.S. Food and Drug Administration (FDA). This document contains a summary of the findings and a proposed design for the next study.
After a thorough review of the proposal and approval of the FDA, the candidate vaccine will undergo three phases of human testing:
Phase I trials
In Phase I, the vaccine is administered to a group of fewer than 100 people. Should the vaccine be intended for children, it will first be tested on adults, then gradually step down the subject age until they reach their target. The goal is to determine the safety of the candidate vaccine and the various responses it triggers in the test subjects.
These trials are non-blinded, meaning that researchers, and sometimes, subjects, are aware if either a vaccine or placebo is administered. A few use the human challenge model—a version of the study that attempts to infect participants with the pathogen after vaccination. In some cases, a modified version of the pathogen is used for the test.
Phase II trials
In Phase II trials, the test subject pool increases to hundreds. A certain number of participants may include those who are more prone to acquiring the disease. The trials are now randomized and controlled, with a distinct placebo group.
Testing is now focused on finding more information on the vaccine’s safety and immunogenicity, as well as proposed doses, immunization schedules, and vaccination methods.
Phase III trials
Following the candidate vaccine’s success in Phase II trials, it moves on to the final phase. Here, the vaccine will be administered to tens of thousands of people to further measure its safety and effectiveness since rare side effects may not appear in smaller test groups.
Phase III tests are randomized and double-blind. They also involve the candidate vaccine being tested against a placebo, which may be a saline solution, a vaccine for another disease, or other substances.
4. Regulatory Review and Approval
Once the vaccine successfully passes through all the phases of clinical trials, the vaccine developer will submit a Biologics License Application (BLA) to the FDA. From there, the FDA conducts an inspection of the manufacturing facility and approves the license.
5. Manufacturing
Major drug manufacturers provide the necessary infrastructure, personnel, and equipment for mass-producing the vaccine. The FDA continues to monitor the vaccine production by inspecting facilities and reviewing the manufacturer’s tests for vaccine potency, safety, and purity, as well as conducting its own testing, in some cases.
6. Quality Control
Even after the approval and distribution of the vaccine, there are systems in place to ensure that it is performing as expected. These include Phase IV trials, which are optional studies that are conducted post-release of a certain vaccine. These systems allow the Center for Disease Control (CDC) and the FDA to continuously monitor the vaccine’s performance, safety, and effectiveness.
Ingredients of a Vaccine
Vaccines are composed of several ingredients which serve a specific purpose, such as providing immunity.
For immunity
Antigens
Antigens are a minute amount of weakened or inactivated pathogen or infectious agent that causes diseases. These are used to help the immune system identify sources of infection and fight them off more effectively.
Adjuvants
This ingredient assists the immune system in responding more strongly to an administered vaccine. It also strengthens the body’s immunity against the disease.
For safety and longevity
These help the active ingredients to remain stable while the vaccine is being made, stored, and transferred. Sugar and gelatin are the common stabilizers that keep the active ingredients intact from temperature shifts and the like.
Thimerosal and other similar substances protect the vaccine from fungus or outside bacteria. These are commonly used in vials of vaccines containing more than one dose. Single-dose vials do not have preservatives.
These ingredients are necessary in the production but are removed from the final product. Miniscule amounts often remain in the vaccine but are harmless.
This aids in the growth of the antigens for the vaccine. Eggs are an example of cell culture material.
These are used to weaken or kill the viruses, bacteria, or toxins in the vaccine. Formaldehyde is one such ingredient.
These prevent the growth of outside germs and bacteria in the vaccine. Neomycin is a common antibiotic added to vaccines.
Types of Vaccines
Live, attenuated vaccines
These are created using weakened ”wild” viruses or bacteria—also known as attenuated—before being included.
Once administered to a person, the weakened antigens replicate within the body. The dose is small enough not to cause diseases in people with healthy immune systems, but can still stimulate an immune response. While rare, a live, attenuated vaccine may cause a milder form of the disease it is immunizing against.
An example of this is the smallpox vaccine. Rather than contain the variola virus–the cause of smallpoxーit contains an attenuated version of a closely-related virus called vaccinia. Since the eradication of smallpox, it is now used to protect researchers who work on the variola virus and other viruses in the same family.
Inactivated vaccines
Inactivated vaccines are created using a killed or inert version of the ”wild” viruses or bacteria. These samples are grown in a culture medium and inactivated prior to being used in the vaccine.
Because the antigen is inactive, this type can be safely administered to immunocompromised individuals. However, they might not develop the same level of immunity as non-immunocompromised people would. Inactive vaccines also typically require booster shots to provide ongoing immunity.
The polio vaccine is an inactivated vaccine. Polio infects a person’s brain and spinal cord, causing paralysis. Knowing this crippling and potentially lethal effect, the polio vaccine uses the inactivated virus that does not affect the recipient.
Toxoid vaccines
This vaccine uses a pathogen’s toxin that causes a specific disease. Through vaccination, the recipient becomes immune to the disease-causing parts of the bacteria or virus, instead of the pathogen itself. In turn, the immune response is targeted towards the toxin rather than the pathogen as a whole.
Diphtheria and tetanus (as part of a DTP combined immunization) are made by inactivating the specific toxins from their corresponding bacteria. This process transforms them into ‘toxoids that, when administered, cause an immune response without leading to the disease. Like inactivated vaccines, toxoid vaccines require booster shots to provide ongoing protection.
Subunit/Conjugate vaccines
In the case of some diseases, a specific protein or carbohydrate can be isolated from the pathogen. These components are used to make the vaccine, which trains the recipient’s immune system to react without inducing sickness. This significantly lowers the chances of an adverse reaction, as only a fragment of the original bacteria or virus is administered.
The influenza vaccine is an example of a subunit/conjugate vaccine. As flu viruses are constantly changing, researchers predict which flu strains will become the most common in the upcoming season. From there, they manufacture a vaccine that covers 3–4 possible strains.
While it is possible that the season’s strains will not be covered by the vaccine, it may still provide some protection.
Prevention is Better than Cure
One of the best ways to answer the question of how to avoid getting sick is to minimize or eliminate the possibility of infection. Vaccination trains the body’s immune system to identify and combat viruses and bacteria effectively, preventing the sickness before it manifests.
For more information on immunization against diseases and other health concerns, contact Makati Medical Center’s HealtHub today.